Our Schroth program at Scoliosis 3DC® is unique in that it is based on original Schroth principles but designed for the modern age. That said, the protocols we use, and have used for years now, are evidence-based, effective treatment options for juveniles, adolescents and adults with scoliosis and/or kyphosis. Patients of all ages and Cobb angles (mild, moderate, or severe) have benefited from our program.
Since the creation of the Schroth Method nearly 100 years ago, life has changed. Patients are busy. Kids and their parents are busy. People want and need the least complicated, most efficient path possible–with the best results!

The Schroth Program at Scoliosis 3DC®
When the Schroth Method was created it catered to patients with very severe curves, often greater than 80°. Patients with this type of severe scoliosis did many supine (lying on the back) and prone (lying on the stomach) floor exercises to reduce the effect of gravity on the spine.
Luckily, over the years, improved scoliosis awareness has led to earlier detection and treatment. While we’ve kept the same concepts, the Scoliosis 3DC® program is designed to be simpler, yet comprehensive. This is so that patients can incorporate their curve-pattern-specific scoliosis exercises into their day–five minutes here, ten minutes there and then a longer exercise session for those who need more focused intensity. We evaluate and asses so that we can teach you the most effective Schroth method exercises for your particular curve pattern. Today, we incorporate more upright exercises, like our patient on the rock, and also add other components for the full 3DC (three-dimensional correction) experience. These upright exercises are more effective at engaging the spinal musculature.
Other amendments include exercises to address the sagittal plane, maneuvers to increase flexibility and strength (mobilizations), streamlined 3D Schroth breathing exercises, and added postural re-education (ADL training)–a powerful tool for curves small or large which can become second nature with practice(1). Compared to another Schroth programs, the way we teach uses far fewer props, making exercise set-up less cumbersome (i.e. more user-friendly). All the above-mentioned changes now allow treatment to be delivered on an outpatient basis for a shorter duration than in years past. Most of our patients participate in twelve-hour programs over four days.
Dr. Marc Moramarco, founder of Scoliosis 3DC®, has been trained by the Who’s Who of Schroth Instructors. His longstanding clinical work with patients has shown he and his team what works, and what doesn’t so they are able to help each patient return home with the most effective program possible for their unique curve.
“Our Schroth protocols and updates are simpler for the patient to put into practice immediately. We can instruct a patient, send them to lunch, and they can sit and eat in their newly modified posture in a way that works to counteract progression. It’s a huge win for the patient!”
– Dr. Marc Moramarco
Schroth has documented results including improved Cobb angle measurements (2-4), improved posture (4, 5), a reduction or elimination of pain (6), improved vital capacity and chest expansion (7-8), and improved self-concept (9). and documented internationally (8, 10-14).
The Scoliosis 3DC® Program
At Scoliosis 3DC®, our evidence-based program focuses on educating, enabling and empowering each patient to take an active role in managing their scoliosis. Our program is modeled after the German model of immersion training, which has been used successfully for decades. Schroth breathing is a nuanced technique. We find it is best taught in multi-hour sessions as originally intended (not one hour here and there). Immersion training is more efficient as patients benefit from experiential learning. This leads to less confusion later on as the longer sessions allow plenty of time for learning, questions, and repetition. Patients are also able to gain the needed skills right away instead of going through long-extended instructional time frames. This is especially important for kids because scoliosis doesn’t wait!
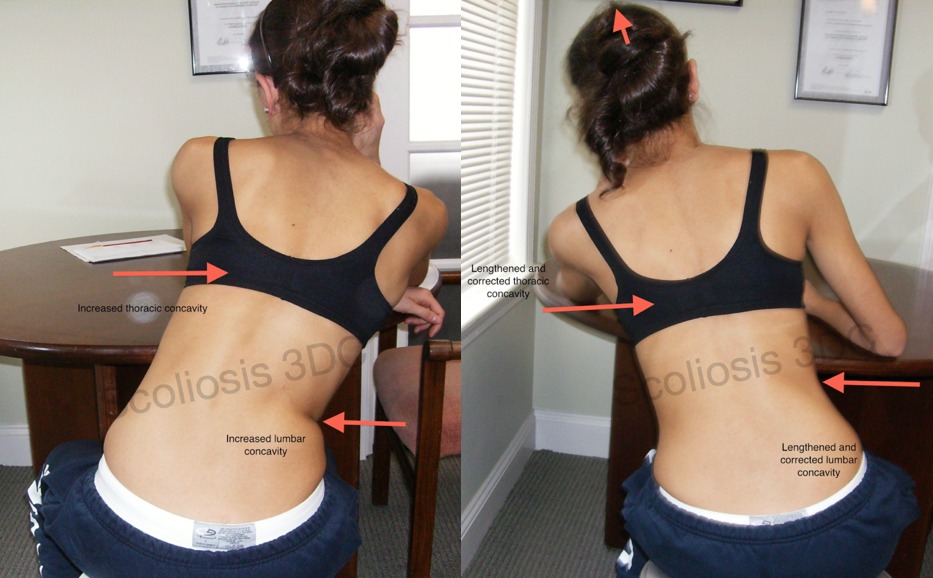
The Scoliosis 3DC® program incorporates load-altering protocols, which allow patients to effect postural control via self-correction (15) during various activities of daily living (ADLs). This enables patients to more easily internalize their newly formed posture and process it as a motor engram (think recoding the brain through repetition). The purpose of self-correction is so the new postures become second nature. This helps to avoid scoliosis progression by not feeding into the curvature during everyday actions. An important component of self-correction used in many of our exercise protocols is the side-shift technique (a lateral trunk shift to the concavity of the curve), which has been shown to be effective in treating scoliosis (16).
Core Components of the S3DC Program
- Customized Treatment – All patients seen in our office are given personalized 1-on-1 attention during their appointments. Each program begins with an examination, during which Dr. Moramarco provides a treatment plan. While every case is different, patients will typically complete a 12-hour program (mild curves, kyphosis, post-surgical, juveniles) or a 17-hour program (moderate-severe curves).
- Patient Education – Extensive education about scoliosis and your/your child’s unique curve pattern (in all 3 planes).
- ADL Training (Activities of Daily Living) – Learn which postures are favorable or unfavorable and why (17) so you can avoid feeding into curve progression when sitting, standing, walking, lying down, carrying objects, and doing regular activities. (These actions add up when repeated many times throughout your lifetime!)
- Sagittal Plane Exercises – Exercises that help mobilize and correct postural imbalances in the sagittal plane– validated by research (18, 19).
- Mobilizations – Simple active, passive, and active-assistive maneuvers used to increase spinal flexibility and range of motion. These can be done alone or with the help of a family member.
- Upright Schroth Exercises – A combination of ADLs and rotational breathing. This creates a streamlined Schroth exercise that is simple, powerful, and can be done anywhere. These scoliosis exercises allow patients to practice throughout the day and increase compliance.
- Old School Schroth Exercises – Rotational breathing exercises designed to engage core muscles and lengthen and strengthen in a corrected position, if needed.
- Personalized Exercise Binder and Video – Once you complete the program, we provide a binder with written instructions for all of your exercises, checklists to help keep you on track, and a video recording of your program for you to reference whenever needed.
- Schroth Bracing – If bracing applies to your case, measurement and fitting can be scheduled alongside an intensive Schroth program.
- The Whisper Brace® – a new innovation in scoliosis bracing -coming soon!

When it comes to choosing the right Schroth method program, personal commitment and experience matter. Our team has a combined experience of more than forty years of Schroth teaching experience between them. We are dedicated to helping you along your scoliosis journey for the optimal outcome acheiveable. Click here to learn more about Dr. Moramarco’s expertise with the Schroth method.
Schroth Therapy Book
 “Schroth Therapy: Advancements in Conservative Scoliosis Treatment,” a text providing insights into some of the nonsurgical scoliosis management techniques. Dr. Marc Moramarco, and his wife Kathy, collaborated with 2nd and 3rd generation Schroth family members, to co-author this book – available on Amazon.
“Schroth Therapy: Advancements in Conservative Scoliosis Treatment,” a text providing insights into some of the nonsurgical scoliosis management techniques. Dr. Marc Moramarco, and his wife Kathy, collaborated with 2nd and 3rd generation Schroth family members, to co-author this book – available on Amazon.
Please note: this book was not intended to be a self-teaching guide but an introduction to Schroth principles. There is a chapter on technique; however, we recommend all patients undertake Schroth exercises only after individualized instruction by a certified practitioner.
References
1) Weiss HR, Seibel S. Scoliosis short-term rehabilitation (SSTR) —a pilot investigation. The Internet Journal of Rehabilitation 2010;1.
2) Fusco C, Zaina F, Atanasio S, Romano M, Negrini A, Negrini S: Physical exercises in the treatment of adolescent idiopathic scoliosis: an updated systematic review. Physiother Theory Pract. 2011;27(1):80-114.
3) Weiss HR, Weiss G, Petermann F. Incidence of curvature progression in idiopathic scoliosis patients treated with scoliosis inpatient rehabilitation (SIR): an age- and sex-matched controlled study. Pediatr Rehabil. 2003;6(1):23–30.
4) Otman S, Kose N, Yakut Y: The efficacy of Schroth s 3-dimensional exercise therapy in the treatment of adolescent idiopathic scoliosis in Turkey. Saudi Medical Journal 2005; 26: 1429–1435.
5) Lehnert-Schroth Christa: Three-dimensional treatment for scoliosis. A physiotherapeutic method to improve deformities of the spine. Palo Alto, CA, 2007; The Martindale Press.
6) Weiss HR. Scoliosis-related pain in adults – treatment influences. Eur J Phys Rehabil Med. 1993;3:91–94.
7) Weiss HR. The effect of an exercise program on VC and rib mobility in patients with IS. Spine. 1991;16:88–93.
8) Moramarco M., Fadzan M., Moramarco K., Heller A., Righter S. The Influence of Short-Term Scoliosis-Specific Exercise Rehabilitation on Pulmonary Function in Patients with AIS. Curr. Pediatr. Rev. 2016;12(1):17–23.
9) Weiss HR, Cherdron J. Effects of Schroth’s rehabilitation program on the self concept of scoliosis patients. Rehabilitation. 1994;33(1):31-34.
10) Weiss HR, Klein R. Improving excellence in scoliosis rehabilitation: a controlled study of matched pairs. Pediatr Rehabil. 2006;9(3):190–200.
11) Borysov M, Borysov A. Scoliosis short-term rehabilitation (SSTR) according to ‘Best Practice’ standards – are the results repeatable? Scoliosis. 2012;7:1.
12) Pugacheva, N. Corrective exercises in multimodality therapy of idiopathic scoliosis in children – analysis of six weeks efficiency – pilot study. Stud Health Technol Inform. 2012; 176:365-371.
13) Lee SG. Improvement of curvature and deformity in a sample of patients with Idiopathic Scoliosis with specific exercises. OA Musculoskeletal Medicine. 2014; Mar 12;2(1):6.
14) Moramarco M, Moramarco K, Fadzan M. Cobb Angle Reduction in a Nearly Skeletally Mature Adolescent (Risser 4) After Pattern-Specific Scoliosis Rehabilitation (PSSR). The Open Orthopaedics Journal. 2017;11:1490-1499.
15) Monticone M, Ambosini E, Cazzaniga D, Rocca B. Active self-correction and task-oriented exercises reduce spinal deformity and improve quality of life in subjects with mild adolescent idiopathic scoliosis. Results of a randomized controlled trial. Eur Spine J. 2014 Feb 28.
16) Maruyama T, Matsushita T, Takeshita K, Kitagawa K, Nakamura K, Kurokawa T: Side shift exercises for idiopathic scoliosis after skeletal maturity. Journal of Bone and Joint Surgery (Br) 2003; 85B; Supp 1: 89.
17) Weiss HR, Hollaender M, Klein R. ADL based scoliosis rehabilitation—the key to an improvement of time-efficiency? Stud Health Technol Inform. 2006;123:594–598.
18) van Loon PJM, Kühbauch BAG, Thunnissen FB. Forced lordosis on the thoracolumbar junction can correct coronal plane deformity in adolescents with double major curve pattern idiopathic scoliosis. Spine. 2008;33:797–801.
19) Weiss HR, Dallmayer R, Gallo D. Sagittal counter forces (SCF) in the treatment of idiopathic scoliosis; a preliminary report. Pediatr Rehabil. 2006;9:24–30.

